Podiatry at Green Cross focuses on the assessment, diagnosis, and management of a range of foot and lower limb conditions. Common issues addressed include corns, calluses, fungal nail & skin infections, foot pain, and verrucae.
During your appointment our Podiatrist will warmly welcome you into our clinic and take a thorough medical, surgical, and treatment history to ensure tailored care.
As healthcare professionals we are bound by a strict code of ethics, therefore any details that you disclose during your appointment will be kept in the strictest of confidence.
After discussing your concerns, a comprehensive examination of your feet is conducted to identify any underlying conditions. Treatment options are explained, and personalised care and advice is provided.
This is the treatment you choose if you are looking for an overhaul of your feet.
Podiatrists understand that healthy feet mean a healthy body. Your appointment begins with a luxury foot bath (only available in our Sheffield Clinic). Nails are cut and filed. Hard skin, corns and cracked heels are painlessly removed. Smoothing with a mechanical sander, followed by a luxurious moisturiser.
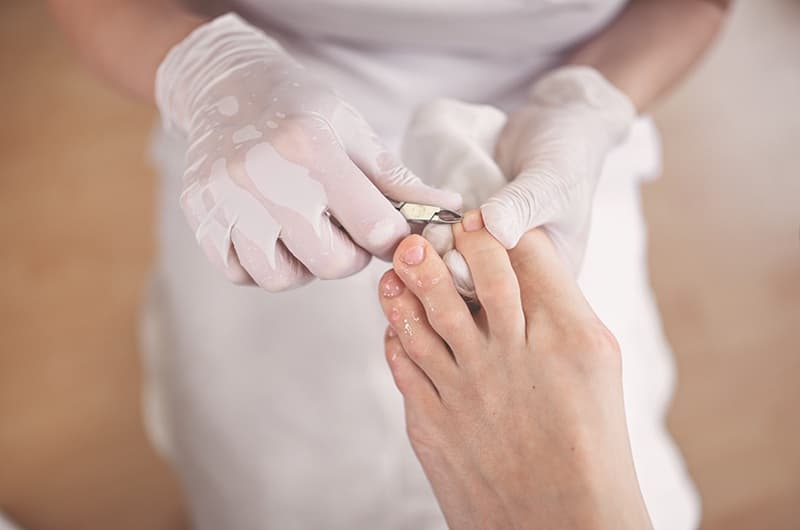
This is for patients who are unable to reach their feet; those taking certain medications or with underlying health conditions that make it difficult to maintain their own nail care.
Our clinic offers a ‘no frills’ treatment to cut and file your toenails and reduce thickening of the nails with an electric drill.
It is especially important to look after your feet if you have diabetes as you are at a much greater risk of developing foot problems.
Overtime raised blood glucose (raised blood sugar levels) can cause damage to the blood vessels and nerves in the feet and legs.
Damage to the nerves can result in the loss of sensation (feeling) in the feet, known as diabetic neuropathy, can lead to the loss of sensation, or the feet becoming numb. Without sensation you may not notice an injury or change in the condition of your feet.
Your circulation may also be affected resulting in reduced blood flow getting to your feet. This can result in slower healing of wounds; pain in your feet or legs; skin and nails can become thin and dry.
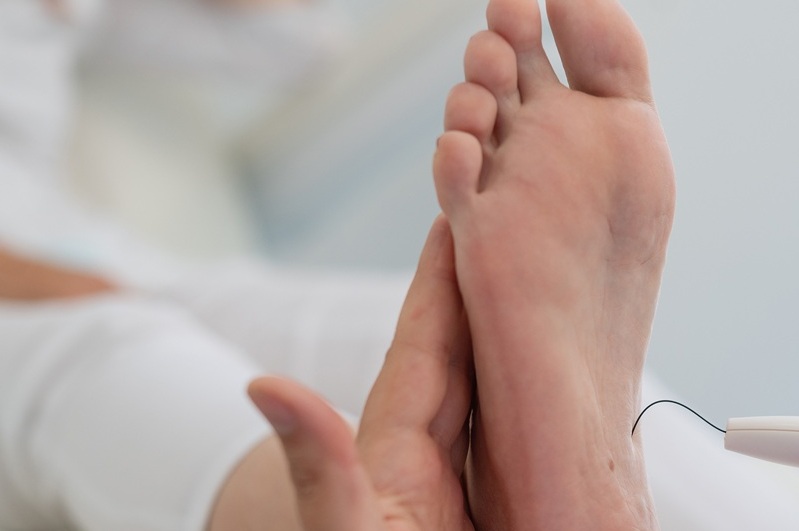
If left untreated foot problems can become serious and may result in diabetic foot ulceration or even amputation.
Most foot problems can be prevented with good, regular foot care. By checking your feet regularly, you will quickly notice any signs of changes to your feet, or any damage that may be occurring and can get help from a healthcare professional to prevent the damaging worsening. Signs of damage can be cuts or grazes, bruising, swelling; changes in colour of your skin; hard skin or ulceration. Also be aware of any cracking from dry skin as this could develop into an ulcer over time.
It is important that people with diabetes have a regular check up with a healthcare professional specifically trained to look after your feet.
Green Cross podiatry & chiropody clinic are able to provide our patients with diabetes not only their annual diabetic foot assessment, but also educate you on how diabetes can affect your feet; develop a treatment plan with advice for a foot care routine you will be able to manage towards having healthy feet in the future.
Are you suffering with painful feet, legs, or hips? If so, then a biomechanical assessment may be able to help you.
A biomechanical assessment examines the lower limbs to find any issues with alignment, structure, weaknesses, or range of motion at joints to help identify your problem. These assessments are suitable for general foot pain; runners, patients with sports injuries, or those experiencing pain/discomfort when they participate in the activities that they enjoy.
During your appointment with our podiatrist a thorough history of your general health and lifestyle will be taken, alongside full details of the circumstance and nature of your foot or lower limb problem.
The podiatrist will undertake a gait analysis, looking at the way you walk, and a ‘hands on’ approach to test the range of motion of the joint of the foot and ankle, and muscle strength of the lower limb, to help to identify links between your symptoms and the position and function of the lower limbs and feet.
Using the findings from your assessment our podiatrist will discuss their diagnosis followed by an effective treatment plan that will include footwear advice, exercises, a rehabilitation program, and/or the possible use of orthotics.
Thick, misshapen, or ingrown toenails can be painful and become infected. Palliative treatment in a podiatry clinic may relieve the symptoms for a short period of time but they often reoccur once the nail starts to regrow.
Nail surgery is routine minor surgical procedure carried out under local anaesthetic, to relieve discomfort from ingrowing and painful toenails, providing a permanent and safe treatment. This is done by removing the offending nail, or part of the toenail and applying a chemical to the root to prevent it from growing back.
A consultation is required before arranging the procedure. Our podiatrists will carry out a thorough assessment and medical history, before explaining the procedure in detail, alongside all pre & post-operative information.
Following nail surgery, you will be required to attend for follow up appointments to assess the healing of the toe.
Verrucas are warts found on the feet, caused by certain strains of the human papilloma virus (HPV). While warts are common and can occur anywhere on the body, verrucae are unique to the feet and are also known as plantar warts.
Though generally harmless, verrucae can cause pain, discomfort, or embarrassment. Studies suggest that many verruca’s resolve naturally within two years, particularly in children, but they may persist in adults without treatment.
Signs and Symptoms:
Verrucae typically cause no symptoms. Some plantar warts can be uncomfortable, particularly if they are present on a weight-bearing area of the foot. ‘Mosaic’ warts (see below) are usually painless.
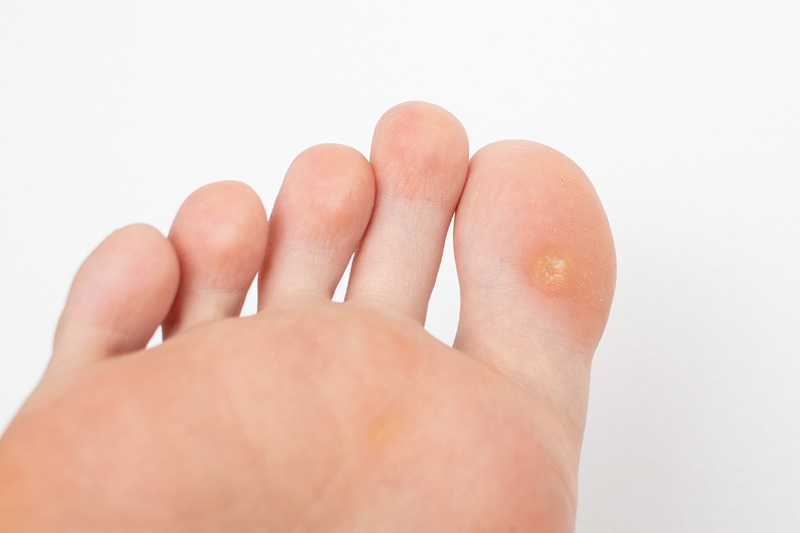
Plantar warts can occur anywhere on the soles and toes, and often affect the weight-bearing areas. They vary in size from just a few millimetres to more than one centimetre. They may have a rough surface that protrudes from the skin surface. On toes verrucae protrude with a cauliflower appearance. Close inspection with a magnifying glass may reveal small black dots.
An individual may have one or many verruca’s, and can also have warts elsewhere on the body. The term ‘mosaic wart’ is used for tightly packed clusters of small plantar warts that resemble a mosaic.
How Are Verrucas Spread?
Plantar warts are caught by contact with infected skin scales, for example from the floors of public locker rooms, shower cubicles and the areas around swimming pools. The virus is not highly contagious, and it is unclear why some people develop plantar warts while others do not. The virus enters the skin through tiny breaks in the skin surface. Moistness and maceration of the skin on the feet probably makes infection with the virus easier.
Treatment
Verruca and warts are one of the most challenging dermatological skin conditions to treat. Treatment selection depends on verruca treatment history, health and age of the patient plus the presentation of the infection. Most verrucae will go away without treatment.
At Green Cross Podiatry, we recommend treatment if verrucae are: Painful, spreading, affecting daily activities, or a cause of significant cosmetic concern.
If a verruca is persistent and does not resolve itself, or if the lesion becomes painful it may require treatment from a podiatrist. At Green Cross Podiatry, we have extensive experience in treating verrucae. We will be able to assess your general medical history and foot health before deciding on a treatment plan. As with any verruca treatment intervention, nothing is 100% guaranteed to be effective, some treatments may work for some patients but not others.
The verruca treatment options we have available in our clinic include:
Debridement
Debridement is the removal of tissue that makes up a verruca as well as any overlying callus.
Debridement is a method of treatment that is used in podiatry to help remove the overlying tissue of a verruca and reduce any associated pain.
Salicylic Acid
This treatment, commonly available in pharmacies in the form of creams, gels, paint, contains a chemical that helps to break down verrucae. Salicylic acid works by softening the infected skin, creating a macerated (soggy) appearance, making it easier for the body to remove the affected cells.
Verrutop
A safe pain free treatment for smaller verrucae and highly effective treatment for children.
Verrutop is a relatively new medication which is used for the treatment of verruca’s and warts. It uses a Nitric zinc complex which is applied to the verruca. Verrutop works by drying up and desiccation of the lesions, which aids cell death. This aids reduction and usually subsequent removal of the verruca.
Those with smaller verruca who want to eradicate them smaller lesions, or verruca/warts which are raised (these tend to occur on the tops of toes or feet usually) are the most suitable to be treated.
Verruca Needling
Verruca needling is a treatment option used for persistent verrucae that are not responding to other treatments. It is around 70% effective six months post procedure which is higher than many other verruca treatment options.
Verruca Needling is a minor surgical procedure carried out under local anaesthetic, which involves the use of a fine needle to puncture the verruca lesion and dermo epidermal junction multiple times. The aim is to implant infected cells into the dermis layer, therefore stimulating an immune response and destruction of the virus.
Curacorn® is a revolutionary treatment where special fillers are injected into the skin to prevent painful, reoccurring lesions such as a callus or a corn. A perfect, long-term treatment for busy people who regularly visit a podiatrist to have them removed or padded using traditional methods. The filler we use is known as Hyaluronic Acid. This is a natural substance which comes with very few side-effects so is even safe to use on patients with Diabetes and Rheumatoid Arthritis.
How does Curacorn® work?
Corns and calluses are formed when there is friction or pressure between the skin and bone. Curacorn® works by injecting the hyaluronic acid between the bone and the outer skin, helping to create a ‘pillow’ effect between the two. This then stops the bodies protective mechanism in the form of callus/corns to the affected area leading to instant pain relief. Simple, right?
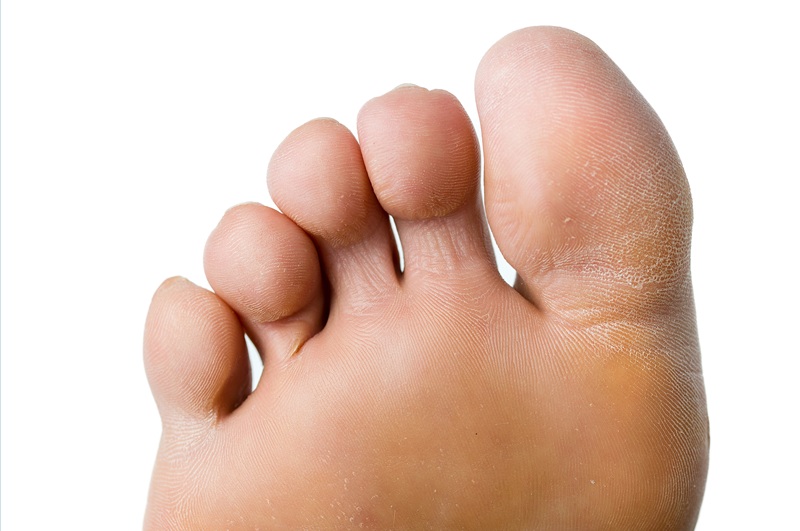
My callus/corn has been there for a long time, can Curacorn® help me?
Yes, Curacorn® is clinically proven to be effective on longstanding callus and all types of corns, including those on the soles of the feet, on top of the toes and also soft corns that lie in-between the toes. In fact, the Curacorn® technique has already been shown to have high patient satisfaction rates for new or reoccurring corns with just 1-2 treatments with its effects lasting up to 18 months or in some cases, longer!
Your Podiatrist will discuss what you can expect from your treatment and how much gel will be needed to create a sufficient cushion inside the skin for you.
Is this painful?
Curacorn® treatment is carried out under local anaesthetic making treatment pain-free! A mild ache may occur at the area of the foot treated for up to 24 hours following treatment so oral analgesic pain relief such as paracetamol are fine to use.
Who can benefit from Curacorn®?
People who can benefit from this unique and innovative treatment include those with: